Introduction
Picture this: It’s a Sunday afternoon. You’ve spent the better part of the morning prepping a gorgeous roast chicken for the family — golden-brown skin, herbs tucked under the breast, the kind of meal that makes your kitchen smell like something out of a Parisian bistro. Everyone sits down, plates are filled, and by Monday morning, half your household is doubled over in agony. The culprit? Salmonella.
It’s the uninvited guest no family gathering needs, and yet, it crashes the table more often than you’d think. The Centers for Disease Control and Prevention (CDC) estimates that Salmonella causes approximately 1.35 million infections, 26,500 hospitalizations, and 420 deaths in the United States every single year. In Canada and the United Kingdom, it remains one of the top causes of foodborne illness — a quiet epidemic that rarely makes headlines until an outbreak forces the issue.
Here’s the good news: Salmonella is one of the most preventable foodborne illnesses out there. You don’t need a culinary degree or a microbiology lab. What you need is the right knowledge — and a handful of habits that become second nature. That’s exactly what this guide is built to give you.
What Is Salmonella, and Why Should You Care?
Before we get into the actionable playbook, let’s get clear on what we’re dealing with.
What is Salmonella caused by? Salmonella is caused by a group of bacteria called Salmonella enterica, most commonly found in raw or undercooked poultry, beef, eggs, and unpasteurized dairy. But here’s what catches most people off guard — it also lurks in fresh produce, contaminated water, and even the mouths and claws of your beloved pets. Yes, your backyard tortoise is a legitimate Salmonella risk.
What are the symptoms if you get Salmonella? The classic triad includes diarrhea, fever, and abdominal cramps — usually appearing 6 hours to 6 days after infection. Nausea, vomiting, and headaches often follow. Most healthy adults recover within 4 to 7 days, but for children under 5, the elderly, pregnant women, and immunocompromised individuals, Salmonella can become life-threatening. The pain tends to be sharp, cramping, and relentless — the kind that makes you wonder if you’ll ever eat again.
Is Salmonella a food poisoning? Technically, yes. It falls under the umbrella of foodborne illness, meaning the bacteria are typically transmitted through contaminated food or drink. However, direct contact with infected animals or humans can also spread it — something far too many people overlook.
What happens when Salmonella enters the body? Once ingested, the bacteria invade the lining of your intestines, triggering an inflammatory response that produces those hallmark symptoms. In severe cases, the infection can break out of the gut and enter the bloodstream — a condition called bacteremia — which is where things get genuinely dangerous.
According to research published in the National Library of Medicine, non-typhoidal Salmonella strains represent a significant global public health burden, particularly in vulnerable populations who may not mount an adequate immune response.
The 8 Ways to Protect Your Family from Salmonella
1. Master the Art of Proper Handwashing
Let’s start with the one that sounds almost insultingly simple — and yet remains the single most effective barrier between your family and a Salmonella infection.
Why it works: Salmonella can transfer from contaminated surfaces, raw foods, or animals to your hands in seconds. From your hands, it’s one casual face-touch or food grab away from entering your system.
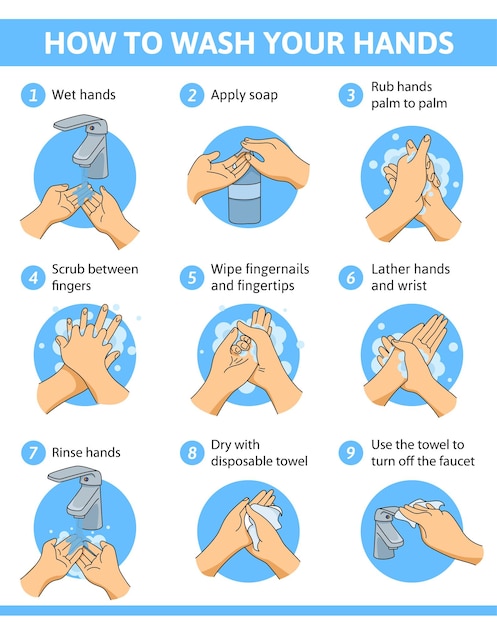
How to do it right:
- Wash hands with soap and warm water for at least 20 seconds — that’s roughly the time it takes to sing “Happy Birthday” twice
- Always wash before and after handling raw meat, poultry, seafood, or eggs
- Wash after touching pets, especially reptiles, amphibians, and baby chicks
- Wash after using the bathroom, changing diapers, and gardening
- Dry hands with a clean towel — not the damp one that’s been hanging by the sink for four days
The Minnesota Department of Health identifies handwashing as the cornerstone of Salmonella prevention — and they’re absolutely right. No fancy gadget replaces it.
2. Cook Proteins to the Right Internal Temperature
Here’s where the thermometer becomes your best kitchen investment — and no, eyeballing whether chicken looks “done” absolutely doesn’t cut it.
Is Salmonella killed by cooking? Yes — heat is one of the most reliable ways to eliminate Salmonella bacteria. The key is reaching the right internal temperature throughout the entire piece of meat, not just the surface.
| Food | Safe Internal Temperature |
|---|---|
| Whole poultry (chicken, turkey) | 165°F (74°C) |
| Ground poultry | 165°F (74°C) |
| Ground beef, pork, lamb | 160°F (71°C) |
| Whole cuts of beef, pork, lamb | 145°F (63°C) + 3 min rest |
| Eggs | Cook until yolk and white are firm |
| Fish and shellfish | 145°F (63°C) |
What temperature kills Salmonella? The bacteria are destroyed at 165°F (74°C). Anything below that is a gamble you really don’t want to take, especially when children are at the table.
Invest in a reliable instant-read digital thermometer and use it every single time. Insert it into the thickest part of the meat, away from bone. It’s a 10-second check that eliminates enormous risk.
3. Prevent Cross-Contamination at Every Step
Cross-contamination is the sneaky villain in most Salmonella stories. It’s how raw chicken juice ends up on your cutting board, then on your lettuce, then in your body — even though you cooked the chicken perfectly.
The rules are straightforward, but they require deliberate habit-building:
- Use separate cutting boards — one strictly for raw meat/poultry, another for produce and cooked foods. Color-coded boards make this effortless
- Never place cooked food back on a plate or surface that held raw protein
- Wash cutting boards, knives, countertops, and utensils with hot soapy water after every use with raw meat
- In the fridge, store raw meat on the lowest shelf, sealed in containers, so juices cannot drip onto other foods
- Sanitize high-touch surfaces — handles, faucets, countertops — especially during food prep
Keystone’s food safety resource points out that many home kitchens inadvertently create cross-contamination pathways during routine cooking, simply because the separation of raw and ready-to-eat foods isn’t maintained with enough discipline.
4. Refrigerate and Store Food Properly
Temperature control is Salmonella management in its most practical form. Bacteria thrive in what food scientists call the “danger zone” — between 40°F (4°C) and 140°F (60°C). Leave food in that range long enough, and bacteria multiply rapidly.
What this means in practice:
- Refrigerate perishables within 2 hours of cooking or purchasing (1 hour if the ambient temperature is above 90°F/32°C)
- Keep your refrigerator at or below 40°F (4°C) — get a fridge thermometer if you don’t already own one
- Never thaw frozen meat on the countertop; thaw it in the refrigerator, under cold running water, or in the microwave if cooking immediately
- Marinate proteins in the refrigerator, never on the counter
- Don’t let leftovers linger in the “danger zone” after a meal
How long can Salmonella live on surfaces? Studies suggest the bacteria can survive on dry surfaces for hours to days, and longer in moist environments. This is why proper refrigeration and surface sanitation go hand in hand.
5. Handle Eggs with Uncommon Respect
Eggs are magnificent — versatile, nutritious, and deeply embedded in the culinary traditions of the US, UK, and Canada alike. They’re also one of Salmonella’s favorite vehicles.
What food is Salmonella found in most often? Raw and undercooked eggs top the list, followed by poultry, unpasteurized milk and juice, raw sprouts, and contaminated fruits and vegetables.
Here’s how to handle eggs safely:
- Buy refrigerated eggs and keep them refrigerated — in the US and Canada, eggs are washed and must be kept cold; in the UK, most eggs are unwashed and vaccinated, but refrigeration is still the safest practice
- Check for cracks before buying and discard any cracked eggs at home
- Cook eggs until both the white and yolk are firm, or use pasteurized eggs for recipes calling for raw or lightly cooked eggs (Caesar dressing, hollandaise, homemade mayo)
- Never leave egg dishes — frittatas, quiches, egg salad — at room temperature for more than 2 hours
- Wash your hands after handling raw eggs
If you love a runny yolk, use pasteurized shell eggs. You keep the experience; you lose the risk.
6. Be Smart About Fresh Produce and Raw Foods
In an era of green juices, raw salads, and farm-to-table everything, it’s easy to forget that fruits and vegetables can carry Salmonella just as readily as chicken. Contamination can happen in the field, during processing, or even in your own kitchen via cross-contamination.
What foods are most likely to carry Salmonella?
- Raw sprouts (alfalfa, bean, clover) — notoriously high-risk because warm, humid sprouting conditions are ideal for bacterial growth
- Pre-cut melons and leafy greens
- Unpasteurized juices and ciders
- Raw or undercooked tomatoes
- Unpasteurized cheeses
How to reduce risk with produce:
- Rinse all fruits and vegetables under running water before eating or cutting, even if you plan to peel them — bacteria on the skin can be transferred inward by the knife
- Scrub firm produce (cucumbers, melons, potatoes) with a clean brush
- Cut away damaged or bruised areas
- Dry produce with a clean paper towel to further reduce bacterial load
- Keep produce away from raw meat in the fridge and on the counter
Raw sprouts deserve a special mention: if you’re feeding young children, elderly relatives, pregnant partners, or immunocompromised family members, cook sprouts thoroughly or avoid them altogether.
7. Manage Pet and Animal Exposure Carefully
This one surprises a lot of families — but it shouldn’t. Animals, particularly reptiles (turtles, lizards, snakes), amphibians (frogs, salamanders), and young poultry (baby chicks, ducklings) are among the most common sources of Salmonella in households with children.
Who is most at risk for Salmonella from animals? Children under 5 are disproportionately affected, as they’re more likely to touch animals and then their mouths, and their immune systems are still developing.
What to do:
- Always wash hands thoroughly with soap and water immediately after handling any animal, their food, or their habitat — hand sanitizer alone is not sufficient here
- Keep reptiles and amphibians out of kitchens, bathrooms, and any areas where food is prepared or eaten
- Don’t let children under 5 handle high-risk animals without very close supervision
- Clean animal enclosures, food bowls, and water dishes outside or in a utility sink — never in the kitchen sink
- If you keep backyard chickens, collect eggs carefully, refrigerate them promptly, and wash hands after every interaction with the birds
Poison Control’s family safety guide specifically flags reptile ownership as a high-risk factor for Salmonella in households with young children — a warning worth taking seriously before adding a tortoise to the family.
8. Know When to Seek Medical Attention
Even with the best precautions in place, infections can happen. The final layer of protection is knowing exactly when Salmonella requires more than rest and hydration.
Will Salmonella go away by itself? In most healthy adults, yes — the infection resolves within 4 to 7 days with rest and adequate fluid intake. But “most healthy adults” is a crucial qualifier.
Seek medical care immediately if you or a family member experience:
- Diarrhea lasting more than 3 days
- Fever above 102°F (39°C)
- Blood in stool
- Signs of severe dehydration — extreme thirst, dry mouth, very dark urine, dizziness, or fainting
- Inability to keep fluids down
Is there a vaccine for Salmonella? Vaccines exist for typhoid fever (caused by Salmonella typhi), which is relevant for international travel. However, there is currently no widely available vaccine for the most common non-typhoidal Salmonella strains that cause the majority of domestic food poisoning cases in the US, UK, and Canada.
What antibiotic kills Salmonella? For severe cases requiring medical intervention, antibiotics such as fluoroquinolones, azithromycin, or third-generation cephalosporins are typically prescribed. However, antibiotic treatment is not always recommended for mild cases and should only be pursued under medical supervision — partly due to growing concerns about antibiotic-resistant Salmonella strains.
What should you eat after Salmonella? Start with the BRAT diet — bananas, rice, applesauce, and toast. Bland, low-fiber foods that are gentle on an irritated digestive system. Avoid dairy, fatty foods, and anything spicy until you’re fully recovered.
Quick-Reference: The Salmonella Risk Table
| Risk Factor | Level | Prevention Strategy |
|---|---|---|
| Raw/undercooked poultry | Very High | Cook to 165°F; use thermometer |
| Raw eggs | High | Use pasteurized eggs; cook thoroughly |
| Cross-contamination | High | Separate boards, surfaces, utensils |
| Pet reptiles/amphibians | High | Handwashing; keep out of kitchen |
| Raw sprouts | Moderate-High | Cook or avoid for vulnerable individuals |
| Unwashed produce | Moderate | Rinse all produce under running water |
| Improper refrigeration | High | Keep fridge ≤40°F; refrigerate within 2 hours |
| Improper handwashing | Very High | 20-second wash at key moments |
Frequently Asked Questions About Salmonella
How do I know if I have E. coli or Salmonella? Both can cause diarrhea, cramping, and nausea, so distinguishing them at home is genuinely difficult. E. coli (particularly O157:H7) more often causes bloody diarrhea and may present without fever, while Salmonella typically includes fever. A stool culture test ordered by a doctor is the only definitive way to tell the difference.
Which is worse, E. coli or Salmonella? Both can be severe. Certain E. coli strains (like O157:H7) can cause hemolytic uremic syndrome (HUS), a potentially fatal kidney complication, particularly in young children. Salmonella can cause bloodstream infections in vulnerable populations. Neither should be taken lightly.
What happens to the body if Salmonella is left untreated? In healthy individuals, the body usually clears the infection on its own. In vulnerable populations, untreated Salmonella can spread beyond the gut into the bloodstream (septicemia), infect the bones, joints, or urinary tract, and potentially become life-threatening.
Can Salmonella infection be cured? Yes. Most cases resolve with rest and hydration. Severe cases are treated with antibiotics. Full recovery is the norm, though some individuals develop reactive arthritis — joint pain, eye irritation, and urinary symptoms — weeks after the infection clears.
What does Salmonella stool look like? Salmonella diarrhea is typically watery, frequent, and may contain mucus. In more severe cases, blood can be present. The color can range from yellow to green, sometimes dark.
How to flush out Salmonella? There is no medical “flush” procedure. The focus is on staying hydrated (water, oral rehydration salts) to replace fluids lost through diarrhea and vomiting, eating bland foods as tolerated, and resting. Antibiotics are used only in severe or high-risk cases.
What are the first stages of Salmonella? The first signs typically appear 6 hours to 6 days after exposure and include nausea, stomach cramps, and the onset of diarrhea. Fever usually follows within the first day.
Is dying from Salmonella rare? For healthy adults in the US, UK, and Canada with access to medical care, death from Salmonella is uncommon. However, globally, and particularly in immunocompromised individuals, the elderly, and young children without access to treatment, mortality rates are significantly higher.
The Bottom Line: Protection Is a Daily Practice, Not a One-Time Event
Salmonella doesn’t announce itself. It doesn’t come with warning labels or visible signs — not on your cutting board, not on your garden-fresh produce, not on the hands that just cuddled the family dog. It operates in the invisible margins of daily life, which is precisely why your defense has to be built into the habits of daily life too.
The 8 strategies outlined here — rigorous handwashing, temperature-correct cooking, disciplined cross-contamination prevention, proper refrigeration, careful egg handling, smart produce management, animal hygiene, and knowing when to seek care — aren’t dramatic interventions. They’re small, consistent choices that compound into powerful protection.
And that’s the thing about food safety: the families who never think about Salmonella are often the ones who have it down to a science. They’ve simply made the right practices automatic.
Whether you’re prepping Sunday roast in London, grilling chicken in Toronto, or making breakfast tacos in Austin, the bacteria don’t discriminate by geography. But your habits can.
Start today. One habit at a time.
Was this guide helpful? Share it with a parent, a partner, or anyone who spends time in the kitchen. And if you want to go deeper on food safety and family wellness, bookmark these trusted resources:
- CDC Salmonella Prevention
- Poison Control: Keeping Your Family Safe from Salmonella
- Minnesota Department of Health – Salmonellosis Prevention
- Keystone: Salmonella Procedures and Tips
- NIH Research on Salmonella
Disclaimer: This article is intended for informational purposes only and does not constitute medical advice. If you suspect a Salmonella infection, please consult a qualified healthcare professional.